I’ve been reporting on Alzheimer’s disease for more than two decades, and any progress in the field has seemed incremental at best, leaving most patients and their loved ones with few options. But in the process of filming a new documentary, “The Last Alzheimer’s Patient,” I met with people all across the country who had been diagnosed with or who are at high risk of the disease. With lifestyle changes alone, I saw levels of amyloid plaque decrease in their brains, their cognition improve and even signs of reversal of the disease.
It was extraordinary and it also made me start to think about my own brain, because I have a family history of Alzheimer’s disease.
So with some trepidation, I decided to learn more about my risk for dementia. It was one of the most personal and revealing experiences I have ever gone through.
To start, I underwent an intensive exploration of my brain, far deeper than I even thought possible. This wasn’t a simple look at the anatomy or even the genetics that might predispose me to a particular type of dementia. The goal was to obtain a complete story of my brain, from my earliest days through my education and formative years to now: a man in his mid-50s. Most importantly, the in-depth testing could give me a clearer idea of where I was headed and how to steer my path in the most favorable direction.
Even as a brain surgeon myself, I was surprised at how well the health of your brain can be measured. With the heart, it is pretty well-accepted that a battery of tests can help give us a clear idea of how to predict, prevent and treat heart disease. Until recently, however, we really could not say the same about the brain. Many brain doctors still struggle even to define the criteria for a healthy brain. The general consensus was that the “black box” in your skull was pretty fixed and that there was little you could do to assess it, let alone optimize it.
Dr. Richard Isaacson, a neurologist, convinced me otherwise, and it led to one of the most fascinating — and somewhat frightening — days I have had in my life. I’ve known Richard for a long time, and we are friends. We have had great conversations about our shared love for the brain, and I often turn to him to get his thoughts on neurological developments in the news. What has always struck me about Richard is that he is consistently unwilling to accept the status quo in medicine, almost more as a matter of justice rather than scientific pursuit, although he is that rare individual who is stellar at making a difference in both.
- Join an NIH-funded study testing software to reduce risk of Alzheimer’s disease.
- Learn more about Dr. Dean Ornish’s peer-reviewed lifestyle research and reversing Alzheimer’s.
- Overview of treatments from the Alzheimer’s Association.
- Mayo Clinic Alzheimer’s Disease Research Center.
So I immediately thought of him when considering the idea of a preventive neurology visit.
To be clear, I wasn’t going to Richard because I thought I had any sort of problem. But that is the point: When people refer to the US medical field as a “sick-care” system instead of a health-care system, this is what I think they mean. Richard would certainly see me if I were sick, but he preferred to see me now, while I was healthy, fully believing he could help me maintain my brain, reduce my chance of dementia and even optimize my function, as he described in a 2018 study.
I flew into Boca Raton, Florida, to see Richard at the Institute for Neurodegenerative Diseases of Florida clinic on a beautiful day in March. He had advised me ahead of time to not exercise or eat that morning and to prepare for a day of intense mental gymnastics. Although this wasn’t an IQ test, he said, in some ways, it would be far more personal.
I must say that it felt very meta to get an assessment of my own brain and find out whether it was functioning as it should or if there were problems I had not yet noticed. Was I getting rusty? Maybe I was making errors that my family, friends and colleagues were too polite to tell me about. If there were gaps in processing speed or executive judgment, they might now be uncovered and unmasked.
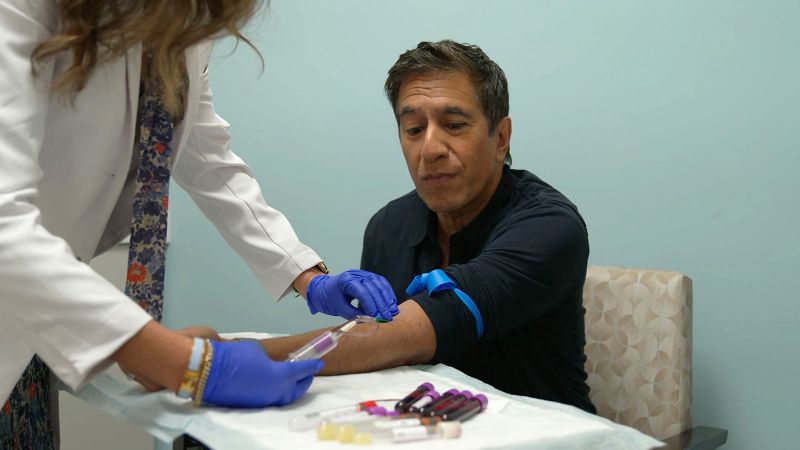
When I got to the clinic, I first underwent a battery of blood tests, checking my phosphorylated tau ratio, better known as the Alzheimer’s blood test, and measures of my lipids, inflammation and glucose levels, to name just a few. I was also tested for my genetic risk for Alzheimer’s. If I was a carrier of the APOE4 gene, it could carry significant higher risk of the disease. I spit into a tube to check my oral health. After that, I stepped on a body composition scale to figure out where and how much bone, fat and muscle I had in my body.
I was a little surprised to catch Richard in the corner, looking at the readout and saying, “Interesting …” while stroking his chin. Nobody likes to see their doctors do that. Not even doctors like to see other doctors do that. “What?” I asked across the room. “Oh,” he replied. “I don’t know, it’s probably fine.” He later told me that he saw evidence of an old left arm injury and accurately predicted that I had had an intense leg workout the day before. It was a real reminder of how clearly the body keeps score. Even though I hadn’t thought about that injury in years, it had clearly left its mark on my body and still triggered a finding on this test.
After that came the cognitive testing. This was perhaps the most surprising. At first, I was told to relax and listen to the detailed short story of an Atlanta football team captain, a quarterback who had injured his finger on a fishing trip before the big game. I thought I had been paying attention but suddenly realized I probably wasn’t as engaged as I thought. “What day did he injure himself, and how many stitches did he need? What was the player’s name?” I was asked 15 minutes later. Could I even be certain if it was his thumb or left ring finger?
Quick: Recite as many words as you can starting with the letter “G” and then immediately rattle off as many animal names as possible, both in one-minute increments. The longer the words and the more unusual the animals, the better. There were lists of words to remember, three-dimensional cubes and clocks to be drawn, and dozens of faces to match with their names. I had to scratch and sniff 50 different smells and determine, in one instance, if something smelled more like gasoline, acetone or a forest fire. In another instance, it was lavender or lilac. I found myself suddenly being unsure and trying to summon up a memory of that smell to try to answer correctly.
I felt like my brain was being cross-examined by a very skilled prosecutor.
It wasn’t just about the number of errors I made but the types of errors, how long I took to respond and whether I simply lost my attention. There are obvious red flags that pop up if someone draws a clock backward or if they have lost their ability to distinguish certain smells. The more subtle concerns were around visual-spatial construction or an ability to ignore incongruent stimuli in the Stroop Color and Word Test, such as identifying the color red, even if that word appears in purple on the screen.
Although I’ve never been diagnosed with dyslexia, Richard thinks it might be something I have. “Do you count on your fingers?” he asked me. I have always done that and never considered it to be notable or suggestive of something significant. Turns out I was less likely to remember words with lots of Bs and Ds in them because I may have always shied away from letters I more easily confused. These types of insights about my own brain, big and small, were all so fascinating (and a bit unsettling) to me. For Richard, however, they represented opportunities for early intervention, some of which are remarkably simple.
“Most doctors would look at your results and say you are doing fine,” Richard explained before he showed me the results of my lab testing. “But what they are really saying is that you are probably fine – for the next few years. I am playing the long game here, and I think you are going to see a lot of areas we can start to address now, today.” I am a pretty competitive guy, so I am used to having all “greens” pop up when I review my lab testing results. After all, I take great pride in my health and approach it with the same rigor that I approached my grades in medical school. I wanted to do really well, certainly as well as I could possibly do.
So when Richard flipped over my lab results and showed me a page that had not only a considerable amount of yellow but even a few reds, my heart dropped.
My homocysteine level was elevated, but my B12 level was low. That wasn’t surprising to Richard, because he had also found a mutation in my MTHFR gene, which meant that I probably didn’t process homocysteine well. My omega-3 levels were all right, but not when you compared them with my omega-6 levels. My DHEA levels were a little low, which might partly explain why I have had more trouble putting on muscle than I did a decade ago. And I was surprised to learn that I was carrying more inflammation in my body than I expected, especially given that I felt fine.
What was most revealing to me was how clearly these blood test abnormalities could be associated with neurological function. Richard told me that issues of metabolism, such as even slight insulin resistance, can accelerate amyloid deposition, which can lead to amyloid plaques, those telltale signs of Alzheimer’s disease, down the line. He also said that, in his experience, cholesterol and lipid abnormalities can be associated with problems with executive function and speed of processing. He added that he associates depression with lower attention and slower processing speeds.
I’ve been practicing neurosurgery for 30 years, and I had never heard of this. Richard was able to draw a link between very functional aspects of the brain to very specific problems in the body. And, more important, he has presented scientific evidence showing that optimizing those physical targets is associated with improved cognitive function.
Richard also wanted to address an activity I did on a daily basis: my neighborhood walk with my three dogs. “Keep doing that,” he said, “but now with a weighted vest.” Why? Not having enough lean muscle mass is problematic. He told me people typically do a good job addressing their arms and legs, but loading the spine with additional weight helps activate core muscles, such as abdominals and obliques, as well as stimulating the growth of new bone cells. This could lead to a critical redistribution of the fat, muscle and bone in my body and help drive down any insulin resistance that I may be genetically predisposed to and eventually lower my risk of developing amyloid in the brain.
On Richard’s advice, I started to make a few changes to my nutrition and day-to-day routine. Over the years, I had gone back and forth on fish oil, not overly impressed with the data on heart health and finding it challenging to keep the pills refrigerated, especially when I was on the road. For Richard, though, it was clear. As healthy as my diet is, he had no doubt that I needed to take the extra steps to supplement with omega-3 fatty acids to help my omega-3/omega-6 ratio in the pursuit of better brain health. This would also help with the absorption of B vitamins, he added. Those needed to be supplemented as well, and Richard was very specific about this. “Make sure to get the bottle with 1,000 micrograms of B12 and 400 micrograms of methylfolate along with 1.5 milligrams of B6.” Those fairly straightforward recommendations to improve my fatty acids could probably make an impact with my executive function, he told me.
In the recommendation about brain health, I did not expect an intervention involving my feet, but the nerves that run to the feet are the longest in our body. When you don’t move your toes and feet regularly and freely, Richard says, you can lose sensory awareness, also known as proprioception, leading to a “sensory paralysis.” Over time, the nerve connections that run from your feet to your brain start to disappear. Once your feet are weak, your weight will be unevenly distributed when walking and exercising. The better your feet can tolerate a load evenly, the more options they have for movement, the better and more cooperative things will be up the chain, including your knees, hips and lower back. Consider wearing toe spacers occasionally, he told me. Start with 10 minutes a day every few days, and increase the time as you get used to them.
Some of the recommendations were more sophisticated. For example, Richard would ideally want even more testing. He’d like to get a detailed DEXA scan of my entire body, not just for bone health but to get a clear look at how much visceral fat I am carrying. Visceral fat is not the subcutaneous fat that you can pinch between your thumb and your forefinger. Rather, it’s the problematic stuff that chokes off the internal organs in your belly. Because visceral fat is so buried and woven into your internal organs, it’s actually quite hard to assess how much someone has. A person could be skinny and still have a lot of visceral fat. Because I had some inflammatory elevations, he worried that I might be one of those people.
He also suggested a brain MRI. He was worried that there might be cerebral blood vessel injury because of a slightly elevated fibrinogen level, a protein that can help the blood clot. The concern was that I might be making more frequent micro clots, which could put me at increased risk of vascular dementia later in life. And finally, a coronary calcium CT scan to detect coronary artery disease at its earliest stages, because as a general rule, what is bad for the heart is also bad for the brain.
To be clear, most of these tests aren’t part of routine care, and I struggle with the cost of it all. They can be expensive and probably wouldn’t be covered by a person’s insurance, especially if they aren’t showing symptoms of Alzheimer’s, dementia or mild cognitive impairment. That is why Richard is also working to make much of it available for free at home. Nearly all the cognitive testing could be available in the future through a free app. Even the blood work could be done via finger-prick testing, if all goes as expected with Richard’s research trial. Although a complete DEXA scan requires a facility, there are home scales that do a reasonably good job at measuring overall body composition, not just weight, and can help follow those trends over time.
When I first visited with Richard after all my testing, I honestly expected to be told I was doing fine – even excellent. That is what every doctor had told me before. But the evidence is clear that when it comes to your brain, prevention and even optimization are possible. We know that in so many areas of medicine, there is a very large white space between being totally healthy and being sick. And it’s an area that a sick-care system would not spend much time addressing, especially if the recommendations are as simple and wildly effective as a few vitamins, toe spacers and a rucksack.
Going through this experience for “The Last Alzheimer’s Patient” was more revealing and jarring than I could have imagined. After all, nobody wants bad news from a doctor, especially when it comes to your brain. But I can take comfort in knowing these tests aren’t laying out a certain future or preparing me for inevitable catastrophe but rather giving me the personalized knowledge that I can use to take action toward a longer, healthier life and a sharper, healthier brain.